Service design for health
Redesigning how care actually feels
Healthcare systems are designed around clinical protocols, referral pathways, and waiting lists — and for good reason. But between the intake form and the discharge summary, there is a person trying to make sense of their situation. Health service design starts with that person.
We work at the intersection of clinical best practice and lived patient experience. That means understanding not just how care is meant to flow, but how it actually feels:
- The confusion of a new diagnosis — when information arrives faster than someone can process it, and nobody checks whether it landed
- The frustration of handoffs — being asked to retell your story to every new team, every new setting, every new intake worker
- The invisible labour of navigation — the phone calls, the forms, the follow-ups that patients and carers manage alone between appointments
We partner with health organisations to close that gap — redesigning services so they work for the people delivering care and the people receiving it.
We partnered with Alfred Mental & Addiction Health to co-design a transformation strategy for the service's future — bringing together frontline staff, senior clinicians, and people with lived experience of mental health and addiction to shape a vision grounded in the reality of care delivery.
Co-design that goes where the care happens
We do not run workshops in a boardroom and call it co-design. We go to the places where care is delivered and received — into waiting rooms, onto wards, alongside intake teams, and into community settings where people are already navigating the system.
Our research is built on three commitments:
- Trauma-informed practice — we design every interaction to minimise harm and maximise agency, especially when working with people in crisis or recovery
- Cultural safety — we work with communities, not on behalf of them, ensuring that the people most affected by a service have genuine influence over how it is shaped
- Clinical governance fluency — we know how to work within the protocols, accreditation frameworks, and decision-making structures that health organisations require
This means our recommendations land in a way that clinical and operational teams can actually act on — not as design provocations, but as implementable change.
When the Centre for Culture, Ethnicity and Health needed to reach young people from refugee and migrant backgrounds with sexual health education during COVID-19, we co-designed a series of educational comics — working with community members to create culturally safe resources that connected to support services and met people where they were.
From mental health wards to primary care waiting rooms
We have worked across mental health, aged care, primary care, sexual health, and hospital settings — each with its own governance, language, and constraints. What connects them is a shared challenge: services designed around systems rather than the people moving through them.
In mental health, that might mean rethinking how a transformation strategy is developed so that people with lived experience are not just consulted but shape the direction. In sexual health, it might mean creating new ways to deliver education that are culturally safe and meet people where they are. In provider-facing systems, it means understanding the daily reality of clinicians who need technology that works at the pace of care, not against it.
- Mental health and addiction services — participatory strategy design with staff and people with lived experience
- Sexual and reproductive health — culturally safe education and outreach for communities often excluded from mainstream services
- Digital health systems — portals and tools that balance strict clinical requirements with the usability clinicians need
- Hospital and aged care settings — service models that work across complex, multi-team environments
Every engagement starts with the same question: what does this service feel like for the person at the centre of it?
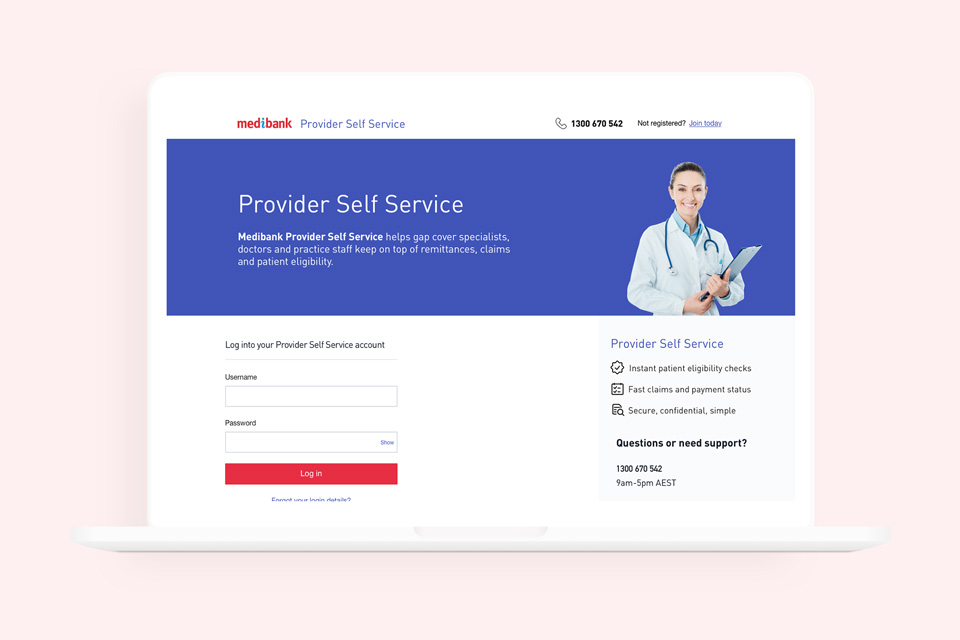
Medibank's Provider Portal was meant to connect specialist clinicians with the insurer, but the experience was falling short. We rethought the portal from the ground up — redesigning the information architecture, simplifying authentication flows, and creating a multichannel communications strategy to guide providers through the transition.
Practical outputs that clinical teams can use
We deliver artefacts that work within the rhythms of healthcare — not design reports that sit on a shelf while the next restructure rolls through. Everything we produce is tested with both the people delivering care and the people receiving it.
What you walk away with depends on the challenge, but it typically includes:
- Patient journey maps — tracing the full experience across touchpoints, from referral to follow-up, surfacing the moments where care breaks down or holds together
- Service blueprints — showing how care flows between teams, settings, and systems, and where handoffs create risk or duplication
- Experience frameworks — giving your organisation a shared language for what good care looks and feels like, grounded in patient and clinician voices
- Implementation roadmaps — sequencing change realistically, working within existing governance structures, workforce realities, and funding cycles
These are tools designed to be picked up and used — by ward managers, by project leads, by the teams responsible for making change happen.
Care that works for everyone in the room
The measure of good health service design is simple: does the service work better for the people who use it and the people who deliver it? Not in a pilot. Not in a presentation. In the daily reality of care.
Our work has helped organisations rethink transformation strategies with the people most affected at the table. It has created new ways to reach communities that mainstream services miss. It has turned provider-facing tools from frustration into utility.
- Staff who feel heard — because the strategy they are asked to implement reflects their reality, not just a consultant's recommendation
- Patients who feel supported — because the service was designed around their experience, not just their condition
- Organisations with a clear path forward — because the roadmap accounts for governance, workforce, and funding, not just aspiration
Health service design is not about making things prettier. It is about making care work the way it should — for everyone in the room.